Can the brain heal itself after a stroke?
The short answer
After a stroke, the brain can reorganize its neural pathways to recover lost functions through neuroplasticity. The best way to promote healing is consistent practice of the affected functions, like deliberately using the weaker side of the body for everyday tasks.
The long answer
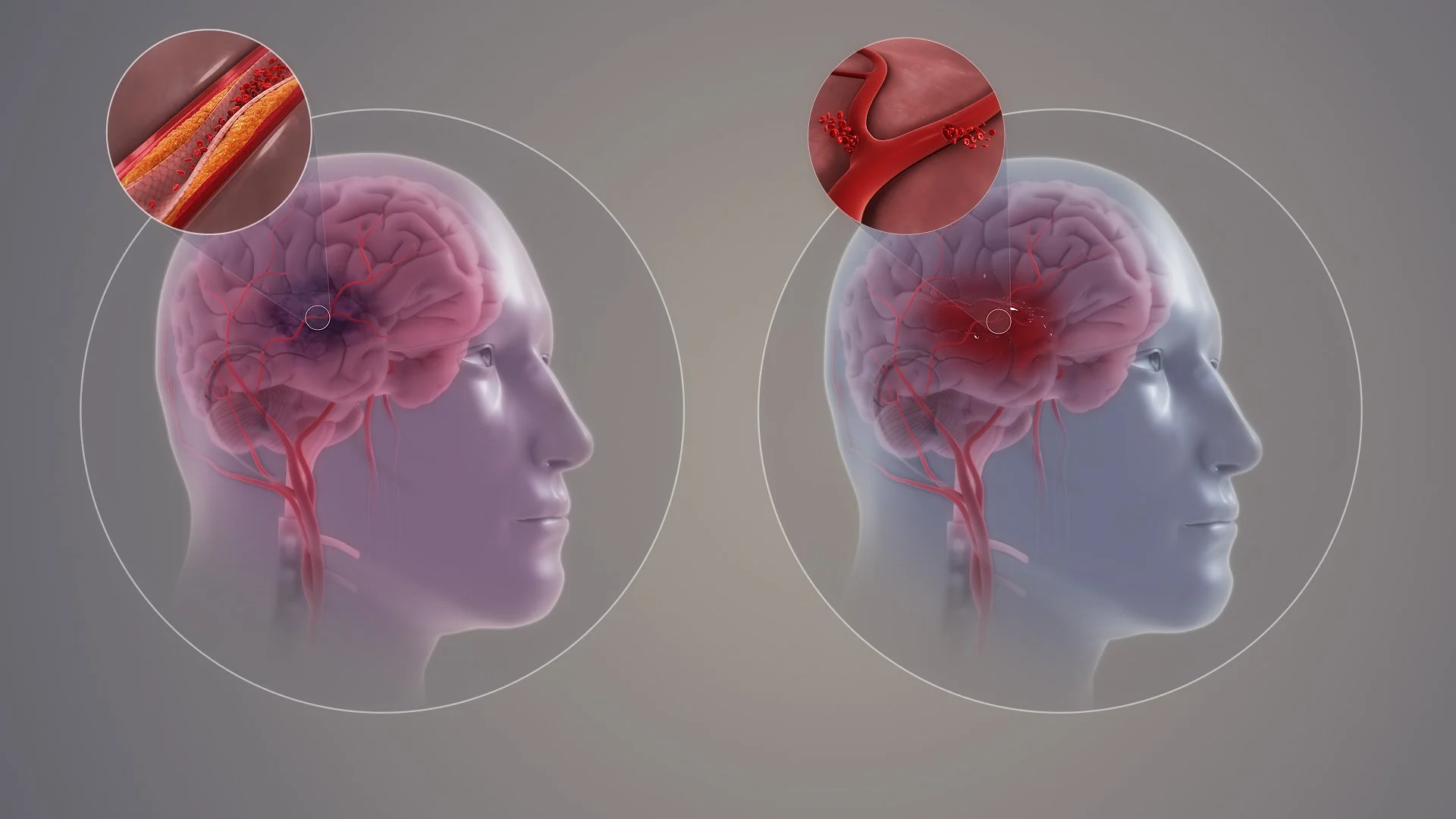
When someone has a stroke, an artery in the brain clogs or bursts. Blood flow stops. And for every minute a stroke goes untreated, 1.9 million neurons die.
This can strip away someone's ability to move, speak, remember — sometimes all three. But when the damage is done, can the brain heal itself after a stroke?
Left: An ischemic stroke is caused by a blocked blood vessel. Right: A hemorrhagic stroke is caused by a burst blood vessel.
"Types of Stroke" by https://www.scientificanimations.com/ is licensed under CC BY-SA 4.0.
Yes, the brain has an extraordinary ability to heal itself after a stroke. But unlike healing a broken bone by rebuilding bone tissue, the brain is not simply creating new neurons (although this happens to some extent). The primary way a brain heals itself is through neuroplasticity.
What is neuroplasticity?
The brain contains billions of neurons, each of which can connect to up to 10,000 other neurons, forming a network of trillions of neural connections. These connections link specialized areas of the brain, enabling perception, movement, and memory.
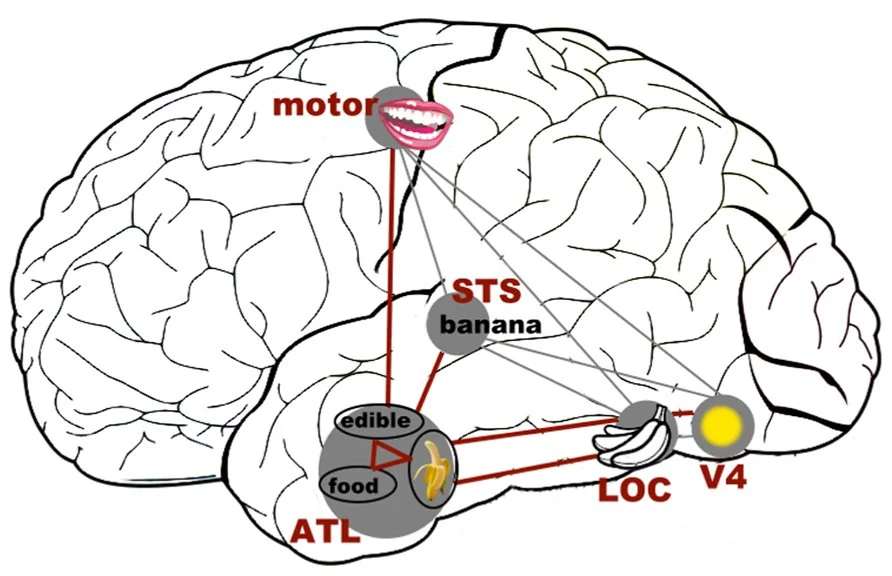
When you see a banana, your brain is piecing together data on the color (yellow), object (banana), and the concept of food (edible).
"A schematic representation of how the (much simplified) concept of a banana as an edible food with its distinct color and shape" by Chiou R and Rich AN is licensed under CC BY 3.0.
Neuroplasticity is the brain's ability to reorganize these neural pathways based on what we learn and experience. While neuroplasticity is always happening, it kicks into a higher gear at certain moments in our lives, like when we're infants and toddlers or after a brain injury.
During the first weeks and months after a stroke, enhanced neuroplasticity allows the brain to form new neural pathways and even transfer functions from damaged sections to healthy areas.
Thanks to neuroplasticity, stroke damage doesn't always result in permanent loss of function. But how exactly does it work?
How does neuroplasticity heal the brain after a stroke?
Neuroplasticity works at two scales: at the level of individual neurons, and at the level of entire brain regions. Here's how both play out.
Mechanism #1: Axonal sprouting and dendritic branching
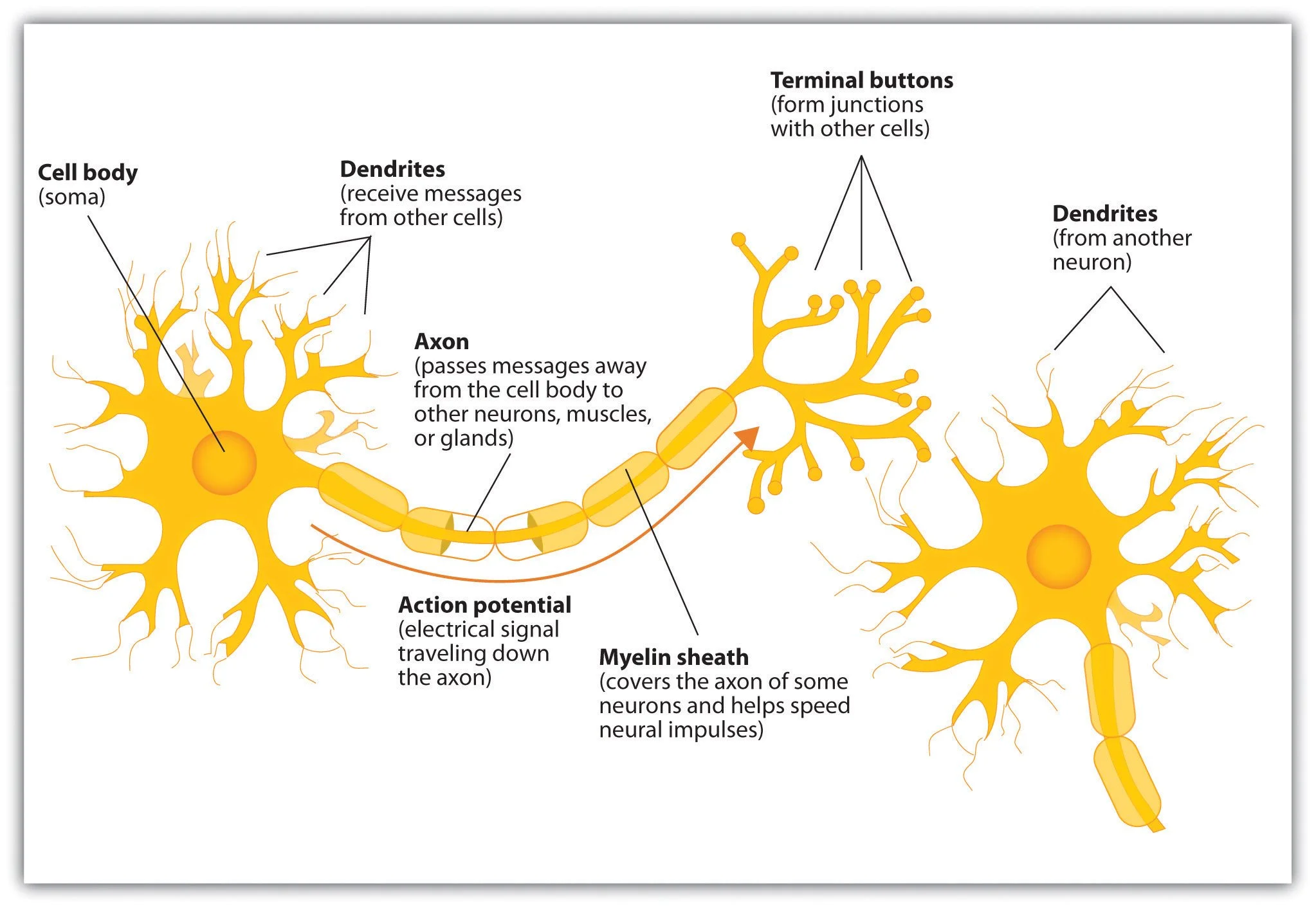
Each neuron has dendrites (which receive messages from other neurons) and an axon (which sends them). During neuroplasticity, these parts experience structural changes to rewire the brain.
"Components of neuron" by Jennifer Walinga is licensed under CC BY-SA 4.0.
With axonal sprouting, the neurons close to damaged areas extend their axons or sprout new axons to try to take over the functions of the damaged neurons.
Axonal sprouting. Source: Post Stroke
Similarly, dendritic branching allows dendrites to grow new branches to form replacement connections. The brain isn't simply creating new neurons from scratch; it's calling on existing neurons to adapt.
Mechanism #2: Cortical reorganization
At a larger scale, the brain can reassign unaffected areas to take over the functions of damaged areas. Neighboring areas of the brain — or even the opposite hemisphere — may take over the jobs of damaged areas.
This happens in non-stroke patients too, like when someone loses a sense. For more on this topic, I recommend reading Livewired: The Inside Story of the Ever-Changing Brain by David Eagleman.
Mechanism #3: Synaptic plasticity
Neuroplasticity also involves strengthening or weakening the connections between neurons based on how often they're used. Put simply, the more we do something, the easier your brain makes it feel.
The clearest example comes from learning: The first time you try playing guitar, it'll feel awkward and difficult. But by the hundredth time you play, it feels natural.
What can a patient do to recover from a stroke?
The best evidence we have to treat post-stroke patients is to actively encourage the brain to rewire itself. The caveat here is that we need to compel the brain to rewire itself positively rather than negatively.
Positive neuroplasticity happens when a patient consistently repeats challenging tasks to build new neural pathways.
Maladaptive neuroplasticity is when the brain rewires itself in an unhelpful way, reinforcing bad habits or compensatory movements that make recovery harder in the long run. In other words, the brain prunes away pathways it sees as unimportant if we're not doing them.
Here are some common post-stroke rehabilitation strategies that encourage positive neuroplasticity.
Constraint-induced movement therapy
Constraint-induced movement therapy examples with the unaffected hand placed in a restrictive mitten.
Source: The Lancet
This technique forces the patient to use the affected limb by restricting the movement of the unaffected limb. The patient will engage motor cortex areas that were affected by the stroke and encourage cortical reorganization.
Constraint-induced movement therapy (CIMT) can significantly improve the motor function of post-stroke patients, even months after the stroke. In a 2006 study, patients who did a two-week CIMT program improved their arm function +34% more than the control group.
Task-oriented training
Source: SingHealth
This rehabilitation involves intentional, repetitive practice of real-world tasks to encourage positive neuroplasticity. For example, if a stroke resulted in limited movement on the right side of the body, a patient should intentionally practice doing things with their right side, like brushing their teeth or picking up a cup. Over time, this will lead to regaining function on the right side.
Speech therapy
Source: Talkshop Speech Pathology
A stroke can affect the muscles we use to speak, as well as the cognitive functions behind finding words and understanding language.
Speech therapy involves targeted exercises to regain motor function, like tongue movements, and language processing practices, like word games. A 2016 study found that stroke patients who received high-intensity speech therapy showed around 70% better language recovery than those who didn't.
Non-invasive brain stimulation
Beyond targeted practice, non-invasive brain stimulation is a promising technique that's been shown to improve outcomes for stroke patients.
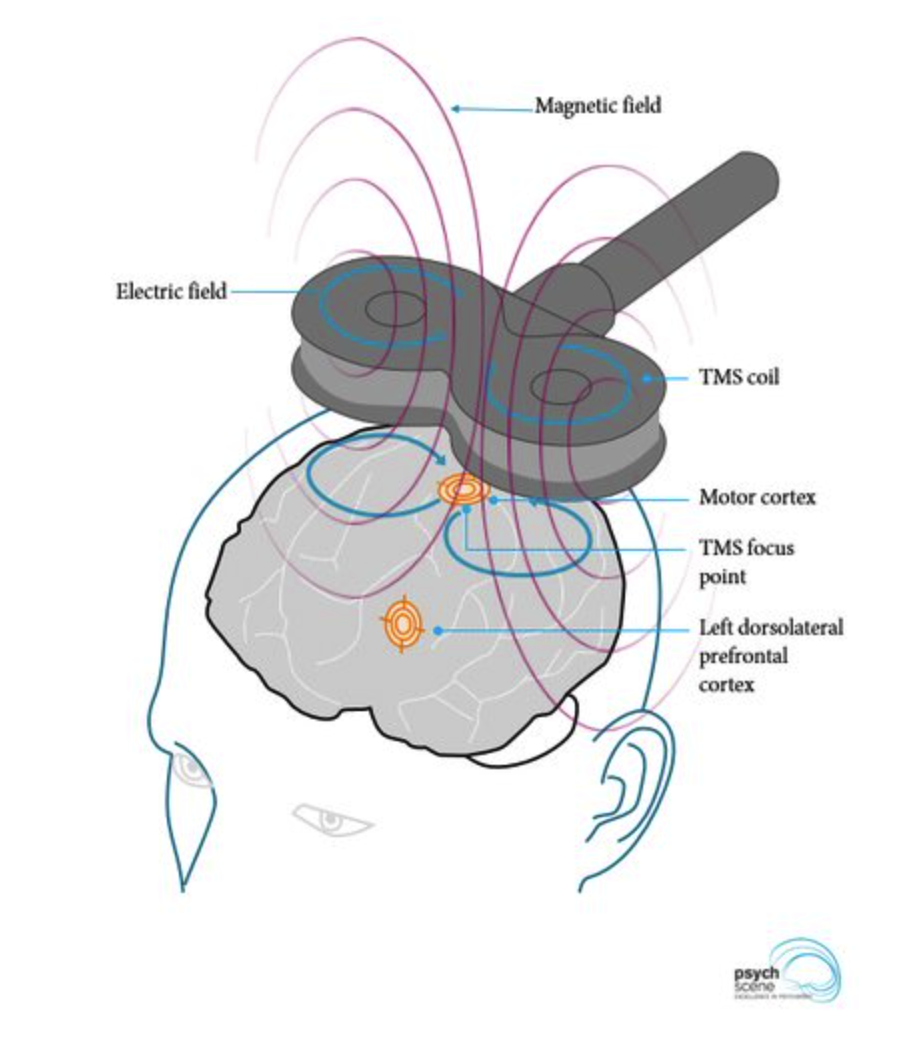
Transcranial magnetic stimulation (TMS) and transcranial direct-current stimulation (tDCS) are outpatient procedures primarily being used to treat major depressive disorder and obsessive-compulsive disorder, but they are also showing promise in stroke patient rehabilitation.
"Transcranial magnetic stimulation (TMS)" by Ilovestarbies is licensed under CC BY-SA 4.0.
These techniques involve using magnetic fields to stimulate neurons (TMS) or low electrical currents to increase or decrease the neural excitability (tDCS). They've been shown to facilitate neuroplasticity by triggering neurons to fire more in affected motor cortex areas or decreasing activity in the unaffected areas, which can interfere with recovery.
While it's not as widely used as other post-stroke therapies, these non-invasive brain stimulation techniques are increasingly being incorporated into rehabilitation programs. One 2012 study found that patients who received TMS had about a 65% chance of better motor recovery than control patients.
Curious about how the world works?
Today You Should Know is a free, weekly email newsletter designed to help you learn something new every Friday.
Subscribe today 👇
Check out some other curious questions:
Sources
Denslow, E. (2023, October 5). Can the Brain Heal Itself After a Stroke? Yes, With Repetitive Practice. Flint Rehab. https://www.flintrehab.com/can-the-brain-heal-itself-after-a-stroke/
Elkind, M. (2007). Faculty opinions recommendation of effect of constraint-induced movement therapy on upper extremity function 3 to 9 months after stroke: The excite randomized clinical trial. Faculty Opinions – Post-Publication Peer Review of the Biomedical Literature. https://doi.org/10.3410/f.1071821.524745
French, B., Thomas, L. H., Leathley, M. J., Sutton, C. J., McAdam, J., Forster, A., Langhorne, P., Price, C. I. M., Walker, A., & Watkins, C. L. (2009). Repetitive task training for improving functional ability after stroke. Stroke, 40(4). https://doi.org/10.1161/strokeaha.108.519553
Hsu, W.-Y., Cheng, C.-H., Liao, K.-K., Lee, I.-H., & Lin, Y.-Y. (2012). Effects of repetitive transcranial magnetic stimulation on motor functions in patients with stroke. Stroke, 43(7), 1849–1857. https://doi.org/10.1161/strokeaha.111.649756
MedLink. (2024, December 9). Neuroplasticity in stroke and brain injury: Shaping modern rehabilitation practices. MedLink Neurology. https://www.medlink.com/news/neuroplasticity-in-stroke-and-brain-injury-shaping-modern-rehabilitation-practices
Newland, E. (2025, March 28). Can your brain heal itself after a stroke? – How to maximize your chances. YouTube. https://www.youtube.com/watch?v=Y2nq6GTpWVw
PAM Health. (2021, November 21). The Benefits of Speech Therapy for Stroke Patients. PAM Health. https://pamhealth.com/resources/the-benefits-of-speech-therapy-for-stroke-patients/
Physiopedia. (n.d.). Neuroplasticity After Stroke. Physiopedia. https://www.physio-pedia.com/Neuroplasticity_After_Stroke
Sakai, K., & Momosaki, R. (2016). Real-world effectiveness of speech therapy time on cognitive recovery in older patients with acute stroke. Progress in Rehabilitation Medicine, 1(0). https://doi.org/10.2490/prm.20160004







We Americans sure do like American things.